- Sep 30, 2024
Intraoperative Neurophysiological Monitoring in Pelvic Floor Surgery
- Fardis Mohiuddin & Faisal Jahangiri
- 0 comments

Pelvic floor surgery is a specialized procedure involving precise maneuvers near critical neural structures, such as the pelvic nerves and muscles. Due to the complex nature of these surgeries, there is a significant risk of nerve damage, potentially resulting in chronic pain or sexual dysfunction for the patient. Intraoperative neurophysiological monitoring (IONM) has been developed in response to these challenges. It is used in surgical procedures to provide real-time feedback on the activity of nerves, allowing surgeons to make informed decisions and minimize the risk of nerve damage during the procedure. This IONM approach has been proven to enhance surgical success and significantly ensure patient safety.
IONM generally involves continuously monitoring neural pathways during surgery to provide real-time feedback to the surgical team. By tracking nerve and muscle activity throughout the procedure, IONM enables the surgical team to immediately notice and address nerve-related problems, allowing for early intervention. In pelvic floor surgery, where preserving nerve function is crucial, IONM plays a vital role. Various pelvic floor surgeries are conducted to correct different pathologies, each targeting specific pelvic problems to enhance patient health. For instance, Pelvic Organ Prolapse Repair addresses the descent of pelvic organs into or outside the vaginal canal. At the same time, Chronic Pelvic Pain Surgery aims to alleviate pain originating from pelvic nerves or muscles. These procedures can significantly improve a patient's quality of life when performed with accuracy.
During these surgeries, IONM utilizes several key techniques, including electromyography (EMG), somatosensory evoked potentials (SSEPs), motor evoked potentials (MEPs), and Pudendal Nerve monitoring with Bulbocavernosus Reflex (BCR). Electromyography (EMG), for example, measures the electrical activity of muscles and provides vital information about their function throughout the operation. Pudendal Nerve Monitoring helps protect the pudendal nerve, an important nerve responsible for bowel, bladder, and sexual functions in the pelvic region.
Monitoring essential neural activity during surgery provides numerous benefits in various medical situations. With real-time feedback, healthcare professionals can perform procedures more accurately, reducing the risk of unintended nerve damage. Moreover, early detection of any neural compromise allows immediate intervention, leading to better surgical outcomes and fewer complications. Surgeons benefit from the confidence of always having the patient’s neural status, enabling them to carry out complex procedures with enhanced accuracy and safety.
While IONM offers significant advantages, it also has challenges, such as the need for specialized technical expertise, the costs associated with the equipment, and the lack of standardized protocols for its use in various surgeries. However, ongoing technological advancements are expected to address these issues and further enhance IONM.
In conclusion, intraoperative neurophysiological monitoring is a valuable tool in pelvic floor surgery. It provides surgeons with real-time feedback and helps to maintain and preserve neural function. By reducing the risk of complications and improving patient outcomes, IONM is advancing surgical practices and improving the quality of patient care. As the technology continues to develop, IONM will most likely play an even more crucial role in ensuring the safety and success of surgeries in the future.
Urethral catheter
A disposable Foley catheter with an embedded bipolar urethral catheter electrode contact for electromyography (EMG) and transcranial electrical motor evoked potential (TCeMEP) recordings. (With permission from Jahangiri et al. Cureus 2019).
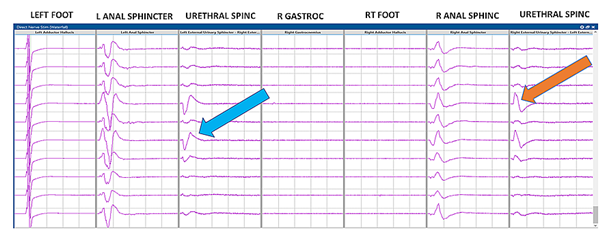
Triggered electromyography (t-EMG) recordings from the urethral sphincter electrodes.
Blue and orange arrows: compound muscle action potentials (CMAP) responses from the external urethral sphincter (EUS). (With permission from Jahangiri et al. Cureus 2019).
References:
Kim, S. M., Kim, S. H., Seo, D. W., & Lee, K. W. (2013). Intraoperative neurophysiologic monitoring: basic principles and recent update. Journal of Korean Medical Science, 28(9), 1261–1269. https://doi.org/10.3346/jkms.2013.28.9.1261.
Schuler, R., Goos, M., Langer, A., & et al. (2022). A new method of intraoperative pelvic neuromonitoring: a preclinical feasibility study in a porcine model. Scientific Reports, 12, 3696. https://doi.org/10.1038/s41598-022-07576-8.
Kneist, W., Ghadimi, M., Runkel, N., Moesta, T., Coerper, S., Benecke, C., Kauff, D. W., Gretschel, S., Gockel, I., Jansen-Winkeln, B., Lang, H., Gorbulev, S., Ruckes, C., & Kronfeld, K. (2023). Pelvic intraoperative neuromonitoring prevents dysfunction in patients with rectal cancer: results from a multicenter, randomized, controlled clinical trial of a NEUROmonitoring System (NEUROS). Annals of Surgery, 277(4), e737-e744. https://doi.org/10.1097/SLA.0000000000005676.
Jahangiri, F. R., Asdi, R. A., Tarasiewicz, I., & Azzubi, M. (2019). Intraoperative Triggered Electromyography Recordings from the External Urethral Sphincter Muscles During Spine Surgeries. Cureus, 11(6), e4867. https://doi.org/10.7759/cureus.4867.
Jahangiri, F. R., Silverstein, J. W., Trausch, C., Al Eissa, S., George, Z. M., DeWal, H., & Tarasiewicz, I. (2019). Motor Evoked Potential Recordings from the Urethral Sphincter Muscles (USMEPs) during Spine Surgeries. The Neurodiagnostic journal, 59(1), 34–44. https://doi.org/10.1080/21646821.2019.1572375.